Authors: Aziz M1,Kamal M2 and Akter S3
Abstract
Background: Self-management of Chronic diseases using digital health technologies have tremendous potential via education, monitoring and support, timely feedback, and remote access to health professionals. The use of digital tools has been surprisingly low in clinical practice, even though the shift to a value-based care system has encouraged the adoption and use of it to manage chronic conditions. Moreover, to our knowledge, there is limited information on the factors that hinder the adoption of digital technologies. Objective: This review provides a comprehensive summary of the barriers to adopt digital health technologies for self-management of chronic diseases which can lead us to develop a model for developing self-management interventions (SMIs) particularly for the developing countries like Vietnam and Bangladesh. Methods: Structured literature searches were conducted using 3 databases to identify relevant studies from 2014 to 2020: PubMed or Medical Literature Analysis and Retrieval System Online, Cumulative Index to Nursing and Allied Health Literature (CINAHL), and Excerpta Medica database (EMBASE). We found 89 literature according to our inclusion and exclusion criteria. The total of 14 articles were included and analyzed using qualitative content analysis. Results: Through the analysis, four main types of barriers for self-management of chronic diseases digitally were found, such as limitations due to personal conditions, inadequate technological competence, poor usability of technology, and hindered motivation to use technology. Conclusions: We can overcome the barriers by real-world testing and incorporating feedback which will help in designing technologies and it will improve their overall usability. Finally, to fully realize the potential of digitally enabled self-management of chronic conditions, there is a greater need to validate these technologies by overcoming these barriers with reliable and accurate information which will improve the cost effectiveness and competency of these digital health technologies. Keywords: Barriers, Self-management, Digital health technologies.
Introduction
Elderly people are growing at a rapid pace as well as the chronic diseases, methods and technologies must be found to help them to take care of their illness by themselves. Self-management of Chronic diseases digitally have tremendous potential via education, monitoring, support, timely feedback, and remote access to health professionals [10]. When designed and implemented successfully digital technology has offered an opportunity to support the quadruple aim of health care by improving health outcomes, increasing patient experience, reducing health care costs, and improving clinician satisfaction. [11]. The American Medical Association defined digital health technologies are as those systems and solutions that engage patients for clinical purposes, collect, organize, interpret, use clinical data, and manage outcomes and other measures of care quality including telemedicine and telehealth, mobile health, wearables, remote monitoring, and apps [12].The use of digital tools has been surprisingly low in clinical practice, even though the shift to a value-based care system has encouraged the adoption and use of it to manage chronic conditions [13]. Moreover, to our knowledge, there is limited information on the factors that hinder the adoption of digital technologies. Previously published literature includes surveys that cite factors influencing Digitalization adoption such as organizational and financial barriers [14]. This review provides a comprehensive summary of the barriers to adopt digital health technologies for self-management of chronic diseases which can lead us to develop a model for developing self-management tools particularly for the developing countries like Vietnam and Bangladesh.
Methods
Structured literature searches were conducted using 3 databases to identify relevant studies from 2014 to 2020: PubMed or Medical Literature Analysis and Retrieval System Online, Cumulative Index to Nursing and Allied Health Literature (CINAHL), and Excerpta Medica database (EMBASE). The detailed search strategies for PubMed have been provided as an example (see Appendix 1). We found 89 literature according to our inclusion and exclusion criteria. At first, two reviewers, with subject matter and methodological expertise, independently reviewed all abstracts identified by the searches and conflicts were resolved by a third reviewer. Then, two reviewers screened the full texts to select the final studies to be included in the review. The authors also conducted a gray literature search (including conference proceedings) through a Web search engine. In addition, one articles were handpicked based on the same inclusion criteria used for articles analyzed using qualitative content analysis. The total of 14 articles were included and analyzed using qualitative content analysis.
Results and Discussion
Through the analysis, four main types of barriers for self-management of chronic diseases digitally were found, such as limitations due to personal conditions, inadequate technological competence, poor usability of technology, and hindered motivation to use technology.
Table I: Key findings of barriers of self-management of chronic diseases digitally.
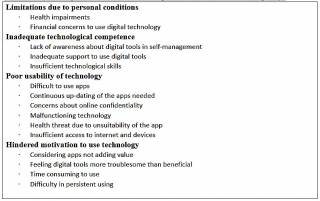
First, Limitations due to personal conditions included health impairments and financial concerns to use digital technology which describes below.
Health impairments contained cognitive and psychological barriers that hinder the use of digital technology in self-management such as creating password, remembering it as well as difficulty to access to the web, which felt like a burden rather help them to manage the diseases (1,3,4). Moreover, physical and sensomotor disabilities impair ability to access to the web and the effort required to use the apps for self-monitor formed a barrier (1, 4).
Financial concerns to use digital technology meant concern about affordability of mobile data (3), affordability of the apps to all (5), concerns about the costs of use of internet (3) and smartphone data plans (9).
Secondly, Inadequate technological competence included lack of awareness about digital tools in self-management, inadequate support to use digital tools, and insufficient technological skills are described in detail below.
Lack of awareness about digital tools in self-management was about limited health literacy (3), information gap about availability of digital tools (2), nor getting recommendation (2) or GP’s advice to use an app (3). Moreover, patients were not being aware of tools available and it was not recommended by their GP or someone else (2, 3).
Inadequate support to use digital tools was about lack of patient education to support self-management as well as they need help to operate the computer (7). In addition, individual needs for additional and expanded training to use smart device system and follow up assistance (6). A study mentioned about the limitations in duration of support (1).
Finally, Insufficient technological skills include Limited skill to use the internet (3), Lack of basic computer skills (3), Difficulty in using apps (5), Inexperience with computer (7), Difficulty in using the net initially as well as later (7) and poor technological literacy (5).
Next barrier for digital self-management is Poor usability of technology which is the most frequently mentioned barrier which includes difficult to use apps, continuous up-dating of the apps is needed, concern about online confidentiality, malfunctioning technology, health threat due to unsuitability of apps and insufficient access to device and internet are described below.
Difficult to use apps includes apps are not user friendly, had complicated layout, and was difficult to use and navigate (5). It also pointed out that different units of measurements in different countries. (5)
Continuous up-dating of the apps needed comprises app content needs continuous re-evaluation for sustainable engagement (8), as well as teaching approach needs reevaluated regularly for sustainable engagement (8).
Concerns about online confidentiality encompasses smart phone base mHealth could pose a threat to unstable patients (6) and Diabetes app doesn’t suit the patients with multiple chronic illness (6). It also mentioned that longitudinal progress on the graph are less useful for patients with stable condition (6) and lack of knowledge to interpret questions of app led to inaccurate report (6). Another study reported that difficult to develop an appropriate PROM [patient reported outcome measures – questionnaire for self-assessment of self- management] (7),
Malfunctioning technology involves technical issues such as connectivity, technology failing, app crash and slow internet connection prevented patients from using DHTs (5). Additionally, some feels that high speed internet is a must (8) for digital health care.
Health threat due to unsuitability of the app covers patients were comfortable with access to health data being limited to only themselves and their providers. However, patients were concerned about personal information is in the web (3, 9), confidentiality of diagnoses (3), and their medication in the web (3). They are also concern about risks of accessing information online (3), vulnerability of online systems to hackers (3), computer viruses (3), and online security (3).
Insufficient access to internet and devices consists of patients have limited access of computers (3), the internet (3,9), and a computer or smartphone (9). It also mentioned that the net and format of the PROM must be easily accessible. (7).
Final barrier is hindered motivation to use technology which includes considering apps not adding value, feeling digital tools more troublesome that beneficial, time consuming and difficult in persisting using described below.
Considering apps not adding value contains patients pointed out current self-care methods were considered sufficient without apps (5), and there is a disbelief that app would improve self-management (5), who feel apps are not superior than writing down physically (5). On top of that, the health condition was not considered to need app for self-care support (5), which makes it less valuable intervention added to the management. Moreover, they assume that their GP is GP is unfamiliar with the technology and not interested about app use (5).
Feeling digital tools more troublesome than beneficial incorporates another barrier frequently highlighted in the literature was the complexity of technologies (n=5). Usability and technical issues led to frustration and discouragement (6) as well as patients have disbelief on help of technology applications in improving quality of life (4). Moreover, they assume that inadequate technical training of health worker may lead to longer consultation (6). In addition, they did not have the desire to learn newer technologies (5). However, patient did not like loss of face-to-face communication (8) because they would not be accountable for their behaviors (2).
Time consuming to use introduces time required to use the apps for self-monitoring formed a barrier (2), as well as intensive assessment, self-survey length and complexity could be burden for patients (7).
Lastly, Difficulty in persistent using have barriers in adapting, persistently using of technology in self- management use (4), as well as sustaining engagement is difficult (8).
Conclusion
Our findings suggest that several important barriers of self-management of chronic conditions digitally such as limitations due to personal conditions, inadequate technological competence, poor usability of technology, and hindered motivation to use technology. Developing countries such as Vietnam and Bangladesh where digitalization is rapidly growing, it will tremendously shape up the health care for the growing elderly population. We can overcome the barriers by real-world testing and incorporating feedback which will help in designing technologies and it will improve their overall usability. Finally, to fully realize the potential of digitally enabled self-management of chronic conditions, there is a greater need to validate these technologies by overcoming these barriers with reliable and accurate information which will improve the cost effectiveness and competency of these digital health technologies.
References:
- Pinchera B, DelloIacono D, & Lawless CA. (2018) Best Practices for Patient Self-Management: Implications for Nurse Educators, Patient Educators, and Program Developers. J Contin Educ Nurs; 49(9):432-440. [doi: 10.3928/00220124-20180813-09.PMID: 30148541]
- Wei P, Shupei Y, & Bree EH. (2016) USA Exploring the Challenges and Opportunities of Health Mobile Apps for Individuals with Type 2 Diabetes Living in Rural Communities. Telemed J E Health; 22(9):733-8. [doi: 10.1089/tmj.2015.0180.]
- Tieu L, Sarkar U, Schillinger D et el. (2015) Barriers and Facilitators to Online Portal Use among Patients and Caregivers in a Safety Net Health Care System: A Qualitative Study. J Med Internet Res; 17(12): e275. [doi: 10.2196/jmir.4847.PMID: 26681155]
- 4. Archer N, Keshavjee K, Demers C, & Lee R. (2014) Online Self-Management Interventions for Chronically Ill Patients: Cognitive Impairment and Technology Issues. Int J Med Inform;83(4):264-72. [doi: 10.1016/j.ijmedinf.2014.01.005. PMID: 2450776]
- 5. Jeffrey B, Bagala M, & Creighton A et el. (2019) Mobile Phone Applications and Their Use in the Self-Management of Type 2 Diabetes Mellitus: A Qualitative Study among App Users and Non-App Users. Diabetol Metab Syndr; 11:84. [doi: 10.1186/s13098-019-0480-4.]
- 6. Kim BY, Lee J. (2017) Smart Devices for Older Adults Managing Chronic Disease: A Scoping Review. JMIR Mhealth Uhealth; 5(5): e69. [doi: 10.2196/mhealth.7141.]
- 7. Holmes MM Stanescu S, & Bishop FL. (2019) The Use of Measurement Systems to Support Patient Self-Management of Long-Term Conditions: An Overview of Opportunities and Challenges. Patient Relat Outcome Meas; 10:385-394. [doi: 10.2147/PROM.S178488. eCollection.PMID: 31908555]
- Reagan L, Pereira K, & Jefferson V et el. (2017) Diabetes Self-management Training in a Virtual Environment. Diabetes Educ; 43(4):413-421. [doi: 10.1177/0145721717715632. Epub Jun 23. PMID: 28643607]
- James D.C.S., Harville C. (2017) Barriers and Motivators to Participating in mHealth Research among African American Men. Am J Mens Health; 11(6):1605-1613. [doi: 10.1177/1557988315620276. Epub Dec 3. PMID: 26634861]
- Morton K, Dennison L, & May C et al. (2017) Using digital interventions for self-management of chronic physical health conditions: A meta-ethnography review of published studies. Patient Educ Couns; 100(4):616-635 [doi: 10.1016/j.pec.2016.10.019]
- Bodenheimer T, Sinsky C. (2014) From triple to quadruple aim: care of the patient requires care of the provider. Ann Fam Med; 12(6):573-576 [doi: 10.1370/afm.1713] [Medline: 25384822]
- American Medical Association. 2016. Digital Health Study: Physicians’ motivations and requirements for adopting digital clinical tools URL: http://tinyurl.com/y67l9zyj [accessed 2019-02-19] [Web Cite Cache ID 76J6gTFIV]
- 13. Mileski M, Kruse C.S., Catalani J, & Haderer T. (2017) Adopting telemedicine for the self-management of hypertension: systematic review. JMIR Med Inform; 5(4): e41 [doi: 10.2196/medinform.6603] [Medline: 29066424]
- Logan AG, Dunai A, McIsaac WJ, Irvine MJ, Tisler A. (2008) Attitudes of primary care physicians and their patients about home blood pressure monitoring in Ontario. J Hypertens; 26(3):446-452. [doi: 10.1097/HJH.0b013e3282f2fdd4] [Medline: 18300854]
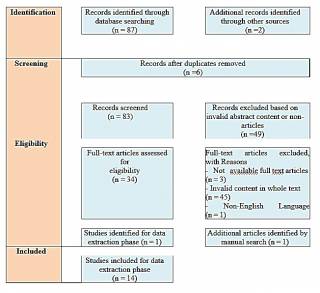
Appendix 1. Prisma diagram for barriers of self-management of chronic diseases digitally.

Thank you for this article. It was very useful. I appreciate the research and effort you put into this post. It shows.
Healthster
27.4.2023 13:34